Community-based peer education as a tool for the prevention of breast cancer: a narrative review
Rachael O Oduyemi1a, Chizoma Millicent Ndikom2b, Gloria Oluwakorede Alao3,4c, Iyanuoluwa O Ojo2d, Faith Ayomide Ajayi5e, Damilola Ajibade6f, Abdullahi Suleiman7g, Hameedah Ayomide Gbadamosi8h and Oluwadamilare Akingbade9i
1Faculty of Nursing Sciences, Chrisland University, Abeokuta, 110104, Ogun State, Nigeria
2Faculty of Nursing, College of Medicine, University of Ibadan, Ibadan, 200001, Oyo State, Nigeria
3Institute of Nursing Research, Osogbo, 232111, Osun State, Nigeria
4Nursiscope Mentorship Academy, Nursiscope Inc., Edmonton, T5Y OW4, Canada
5Ahmadu Bello University, Zaria, 810001, Nigeria
6Chrisland University, Medical Centre, Abeokuta, 110104, Ogun State, Nigeria
7Bayero University Kano, Kano, 7000001, Kano State, Nigeria
8Olabisi Onabanjo University Teaching Hospital, Sagamu, 121101, Ogun State, Nigeria
9School of Nursing, Dalhousie University, Halifax, B3H 4R2, Canada
ahttps://orcid.org/0000-0003-2451-7277
bhttps://orcid.org/0000-0002-4036-156X
chttps://orcid.org/0009-0009-9547-3831
dhttps://orcid.org/0000-0002-2132-2987
ehttps://orcid.org/0009-0006-9928-4294
fhttps://orcid.org/0009-0004-7141-8030
ghttps://orcid.org/0009-0002-0137-6977
hhttps://orcid.org/0009-0002-5771-0559
ihttps://orcid.org/0000-0003-1049-668X
Abstract
Background: Breast cancer remains a major threat to women, especially in low-resource settings like Nigeria, where awareness and screening are limited. Peer education may offer a practical way to improve early detection and prevention in these communities.
Objective: To examine how peer education supports breast cancer prevention in communities by exploring its delivery methods, impact on knowledge and behaviour and the cultural and practical factors that shape its effectiveness.
Methods: A narrative review was conducted to explore the role of community-based peer education in breast cancer prevention. Relevant studies published between 2010 and 2025 were identified through a systematic search of six databases (CINAHL, PubMed, Web of Science, Embase, Medline and APA PsycINFO) using specific keywords. After screening and applying inclusion and exclusion criteria, data were extracted from selected studies and thematically analysed to identify patterns, benefits and challenges of peer education interventions.
Result: Out of 818 studies initially retrieved, only 18 met the eligibility criteria and were reviewed, covering diverse locations and participant groups, mostly from high-income countries. The studies showed that peer education delivered through various methods and tailored to cultural contexts significantly improved breast cancer awareness, screening behaviours and community engagement, though challenges like role confusion, cultural barriers and logistical issues were also reported.
Conclusion: This review concludes that peer education is an effective, adaptable strategy for promoting breast cancer prevention in community settings, especially among underserved populations.
Keywords: breast, cancer, peer-based education, community
Correspondence to: Oluwadamilare Akingbade
Email: oakingbade@dal.ca
Published: 07/04/2026
Received: 11/09/2025
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background
Globally, cancer continues to rise at an alarming pace, affecting millions each year and placing an immense burden on individuals, families and healthcare systems. In 2022, the International Agency for Research on Cancer reported nearly 20 million new cancer cases worldwide, resulting in approximately 9.7 million deaths. Lung cancer was the most commonly diagnosed cancer, followed by breast cancer in women [1].
In Nigeria, the number of new cancer cases increased to 127,763, with 79,542 deaths and breast cancer emerged as the most prevalent, accounting for 25.3% of cases [2].
The uptake in Nigeria on the practice of breast self-examination (BSE), clinical breast examination and mammography remains low due to poor awareness, sociocultural beliefs, limited access and inadequate knowledge [3, 4].
Systemic delays within the health system such as fragmented delivery of health services, shortages in the health workforce, inadequate health financing, weak health information systems and limited access to essential medicines and technologies further worsen outcomes, as most Nigerian patients present at late disease stages. For example, a Northern Nigeria study found 99.4% presented with advanced disease [5], while a review reported symptom durations of 8–12 months before diagnosis [6]. These findings underscore the need for scalable interventions targeting awareness and behaviour at the community level.
Community-based peer education is an approach to health education and promotion in which trained community members known as peers educate and train others within the same community to improve attitude, knowledge and health-seeking behaviour to specific issues. Community-based peer education offers a promising solution. Peer-to-peer models leverage trust and shared experiences to deliver culturally relevant health messages. Successfully used in HIV prevention and adolescent health [7], peer education has also improved breast cancer screening uptake, as seen in Minnesota’s Breast Cancer Champions program [8]. However, evidence from Sub-Saharan Africa is limited. In Nigeria, few studies have applied peer-led models to breast cancer prevention. One study showed peer-led training improved BSE practices among students [9, 10], yet little is known about the cultural adaptation or outcomes of such interventions in rural and underserved communities.
This review will provide context-specific insights into how peer-led education can enhance breast cancer prevention in Nigeria. Findings will guide the design and scaling of culturally appropriate, community-driven programs that strengthen early detection and reduce mortality [7, 8, 10].
This review aims to:
-
To examine the structure, strategies and delivery methods of peer education programs used in community settings for breast cancer prevention.
-
To assess the impact of community-based peer education on knowledge, attitudes and screening behaviours related to breast cancer among women.
-
To identify contextual and cultural factors that influence the effectiveness of peer education interventions in rural and underserved communities.
-
To explore the challenges and facilitators associated with implementing peer-led breast cancer prevention programs.
-
To provide evidence-based recommendations for designing, adapting or scaling up peer education models for breast cancer prevention in similar contexts.
Methods
A narrative review approach was adopted to examine the role of community-based education in breast cancer prevention, as this approach enables a thorough understanding by synthesising a broad spectrum of literature [11]. The study aims to explore and synthesise existing evidence on the role of community-based peer education in the prevention of breast cancer . This narrative review was conducted and reported in accordance with the Scale for the Assessment of Narrative Review Articles (SANRAs). The quality of this narrative review was also assessed using the SANRA, a validated tool designed to improve the methodological rigor and reporting quality of narrative reviews [12]. SANRA consists of six criteria: (1) justification of the article’s importance, (2) clarity of aims, (3) description of the literature search, (4) quality and appropriateness of referencing, (5) scientific reasoning and (6) presentation of relevant data in an organised manner. Each criterion was rated on a 0–2 scale, where 0 indicates low quality, 1 indicates moderate quality and 2 indicates high quality, resulting in a maximum possible score of 12. The current review attained a SANRA score of 12, reflecting clarity of the review objectives, transparent description of the search process, appropriate and consistent referencing, logical synthesis of evidence and structured presentation of findings. The application of SANRA strengthened the overall rigor, transparency and reliability of this narrative review.
Search strategy
A systematic literature search was conducted to identify relevant studies that discussed the utilisation of community-based peer education in the prevention of breast cancer. Six databases were searched including CINAHL, PubMed, Web of Science, Embase,Medline and APA PsycINFO using keywords including ‘breast cancer,’ ‘breast carcinoma,’ ‘breast neoplasm’, ‘mammary cancer’, ‘Breast Neoplasms’, ‘prevention’, ‘risk reduction’, ‘screening’, ‘screen’, ‘breast self-exam’, ‘clinical breast exam’, ‘health promotion’, ‘Primary Prevention’, ‘Early Detection of Cancer’, ‘Mammography’, ‘Health Promotion’, ‘peer education’, ‘peer-led’, ‘peer to peer’, ‘peer support’, ‘lay health’, ‘worker’, ‘lay educator’, ‘community health volunteer’, ‘peer mentor’, ‘Peer Group/education’, ‘Community Health Workers’, ‘Health Education/methods’, ‘community-based’, ‘community setting’, ‘rural community’, ‘village’, ‘low-resource’, ‘underserved’, ‘grassroots’, ‘population-based’, ‘Nigeria’, ‘sub-Saharan Africa’, ‘Community Health Services’ and ‘Rural Health’. Results were exported to the Covidence software for de-duplication and screening.
Interventions and comparisons
The review considered peer education programs aimed at increasing awareness, improving knowledge and enhancing uptake of breast cancer prevention and screening services. Interventions included home visits, group workshops, culturally tailored community education, storytelling, faith-based activities, health fairs and mobile health tools.
Inclusion and exclusion criteria
Studies were included in this narrative review if they focused on community-based or peer-led education interventions aimed at the prevention of breast cancer. Eligible studies targeted women of any age group and were conducted in community or rural settings. The review considered quantitative, qualitative and mixed-methods studies that provided relevant data. Only articles published in peer-reviewed journals, written in English and recently published within 2010–2025 were included to ensure the review captured recent developments and trends in the field.
Studies were excluded if they were hospital-based or focused on clinic-led interventions with no community or peer education component. Articles that addressed types of cancer other than breast cancer, or those that were editorials, reviews, commentaries or opinion pieces or non peer-reviewed studies were also excluded. In addition, studies not published in English or not available in full-text format were excluded from the review. Decisions for data inclusion and exclusion were documented using the PRISMA chart.
Data screening
Title and abstract screenings of relevant papers were conducted according to the established criteria, focusing on the role of community-based peer education in the prevention of breast cancer.
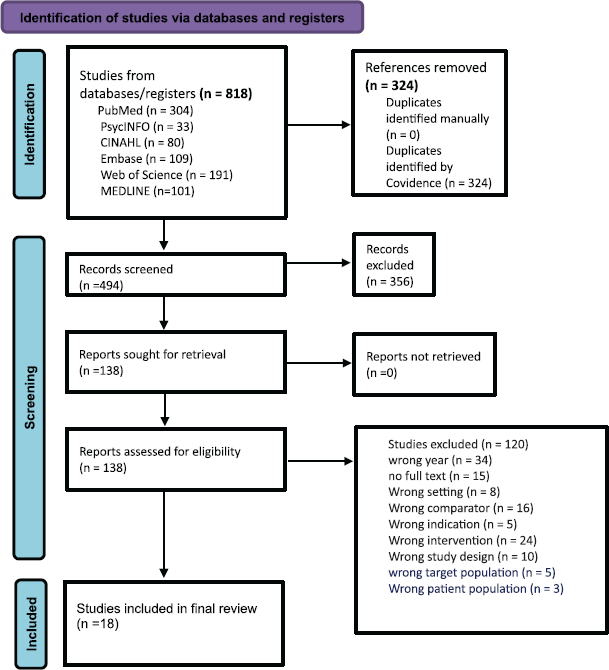
Figure 1. PRISMA flow chart.
Data extraction
Three authors independently extracted data from the selected articles using a data extraction form. This form was developed and pilot-tested on three articles, after which no further modifications were necessary. Extracted information included authors, publication year, study objectives, role of community-based education on breast cancer prevention, benefits, challenges and limitations of community-based education, as well as recommendations for their implementation. To ensure accuracy and completeness, a fourth reviewer verified the extracted data. The collected data were then synthesised thematically to identify patterns, trends and gaps within the literature.
Results
Search results
A total of 818 studies were retrieved from the database search. After removing 324 duplicates, 494 studies remained for title and abstract screening. Of these, 356 studies were excluded, leaving 138 studies for full-text review. Subsequently, 120 studies were excluded for reasons such as publication year, lack of full text, inappropriate setting or wrong target population. Ultimately, 18 studies were included in this review (Figure 1).
Study location
Thirteen (
Study characteristics
Table 1 provides a detailed description of the characteristics of the included studies. The majority (
Study participants
All participants in the included studies were female. The categories represented were African American (
Structure, strategy and delivery of peer education
Peer education in the studies included in this narrative review was implemented through a variety of structures, strategies and delivery systems (Table 2). The selection of peer leaders varied across studies: some were chosen through application and interview processes [25], while others emerged from community-led initiatives [18], community engagement and partnerships [22, 23] or volunteered for the role [26, 28]. In several studies, community health extension workers (CHWs) also served as peer leaders [17, 18, 24, 27]. Regardless of their selection method, all peer leaders received training to prepare them for their roles.
A range of educational materials and tools were utilised to support peer education. These included videos [13, 17, 18, 21], manuals [13, 24], PowerPoint presentations [14, 25] and demonstrations [16, 23, 26, 28].
The delivery methods were equally diverse. Group discussions [17, 21, 22, 23], virtual sessions [13, 27], focus groups [28], house-to-house visits [26] and teaching sessions [16, 22, 24] were all employed to engage participants and facilitate knowledge transfer. The studies demonstrate that peer education can be effectively adapted to different contexts through flexible selection processes, comprehensive training, varied educational resources and multiple delivery channels.
Impact of peer education in the prevention of breast cancer for community-based peer education interventions
Findings from multiple studies consistently demonstrate that peer education significantly enhances breast cancer awareness, knowledge, screening uptake, positive health behaviours and empowerment particularly in underserved communities (Table 3). For example, study by Ahmad
Table 1. Geographic distribution, objectives and focus areas for community-based peer education interventions.
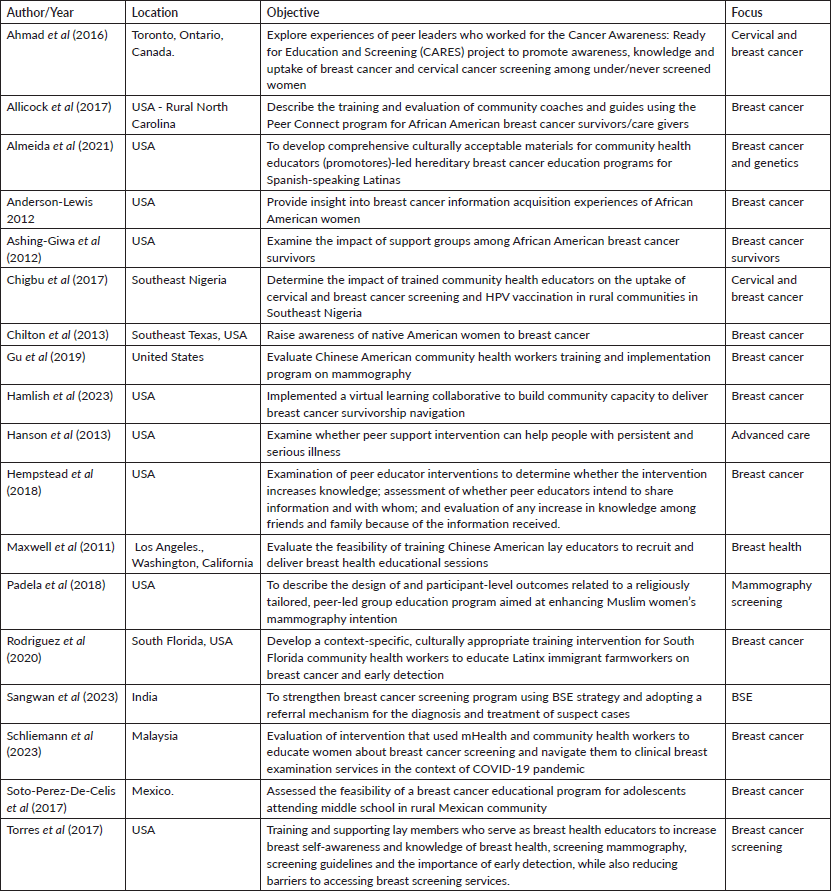
Table 2. Study design, target groups and delivery approaches for community-based peer education interventions.
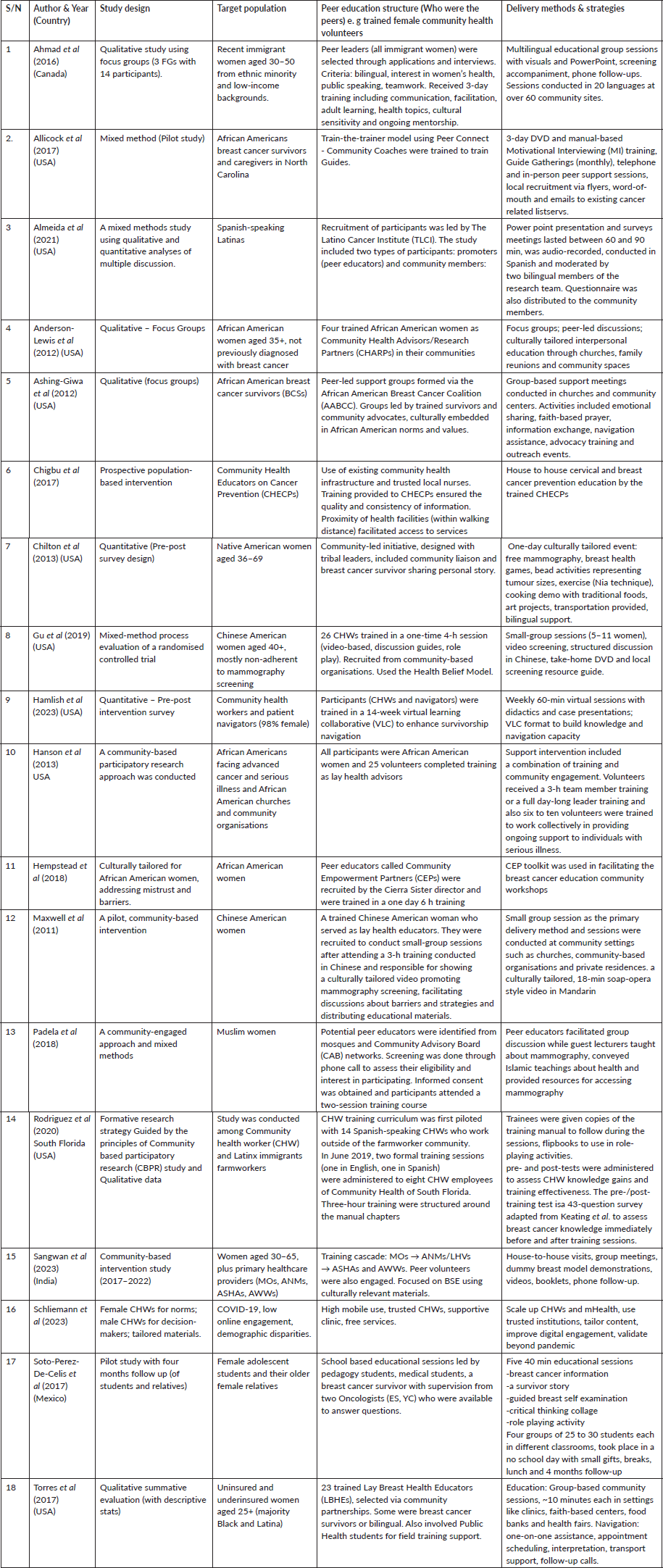
Table 3. Outcomes, contextual influences, implementation barriers and enablers and key recommendations.
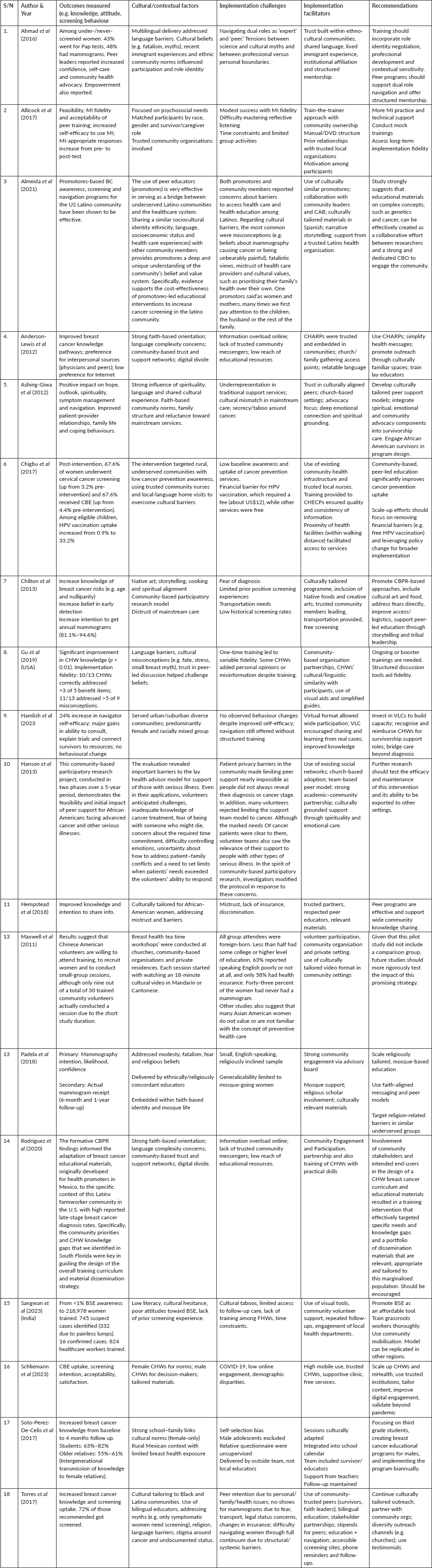
Culturally tailored peer-led interventions also yielded positive outcomes in Native American populations; findings reported an increase in the intention to undergo annual mammography from 81.1% to 94.6% [16]. Likewise, there was documented improvements in spiritual well-being, hope and patient-provider communication among African American breast cancer survivors who participated in peer support programs [15].
Regarding follow-up, studies by [23, 25, 26] monitored participants using phone calls, while [27] conducted a 4-month follow-up. These follow-up strategies likely contributed to the observed increases in screening uptake.
Challenges and facilitators associated with peer education approach
Despite promising outcomes, several challenges were identified across the studies. Rodriguez
Several facilitators enhanced the effectiveness of peer education programs. A key factor was cultural and linguistic alignment between educators and participants, which fostered trust and relatability, as reported by [14, 17]. Programs grounded in faith or cultural traditions, such as those described by [12, 22], benefited from community familiarity and moral authority. The use of culturally tailored tools including bilingual videos [21], storytelling and art [16] and breast models for demonstration [26] further supported effective learning. Additionally, comprehensive training and mentorship, as demonstrated by [24, 25], equipped peer educators with practical skills and structured educational materials, enhancing program delivery.
Factors influencing effectiveness of peer education
Community-based peer education interventions have proven highly effective in promoting breast cancer prevention among underserved women in diverse settings. A key factor was cultural and religious alignment between peer educators and participants, which fostered trust and helped overcome barriers like modesty, fatalism and stigma [15, 22, 23], Faith-based programs, such as mosque-centered education, notably increased women’s willingness and confidence to seek screening.
Language adaptation and literacy-sensitive approaches were also vital. [26] reached over 218,000 rural women using local languages, visual aids and storytelling, identifying numerous suspect cases. Similarly, [14, 25] found that materials tailored for low-literacy audiences improved understanding and retention.
Trust and community embeddedness consistently boosted participation. Engaging respected local figures, including breast cancer survivors and community health workers, led to substantial increases in screening uptake. For example, [29] reported cervical cancer screening rates rising from 3.2% to 67.6%, and clinical breast exams from 4.4% to 67.6%. Padela
Effective training and ongoing mentorship enhanced peer educators’ knowledge and program adherence [17, 25]. Practical support, such as free screening, transport assistance and community-based sessions further increased participation, especially among low-income women [16, 29].
While cultural and behavioural factors are critical in shaping the effectiveness of peer education, system-level determinants also play a significant role in influencing outcomes. The availability and accessibility of early detection and diagnostic services, proximity of health facilities, cost of screening or treatment and trust in healthcare providers can all impact whether participants are able to act on the knowledge and motivation gained through peer-led interventions. Studies showed that even when peer education successfully increases awareness and intention to screen, structural barriers such as transportation challenges, financial constraints and limited healthcare infrastructure can limit actual uptake of services [23, 26, 28]. Integrating these system-level considerations into program design through strategies such as mobile clinics, subsidised screening, navigation support and partnerships with trusted healthcare providers can enhance the reach, uptake and sustainability of peer education interventions across diverse contexts.
Recommendations for designing peer education model
The studies included in this review offer several key recommendations for designing effective peer education models. First, lay health community-based programs should be integrated with strong collaborative partnerships within the community to enhance reach and acceptance [12, 23]. Peer education should incorporate multicomponent community education and navigation interventions to encourage positive health actions, often leveraging religious concepts to increase relevance and engagement [22, 27].
A train-the-trainer approach is recommended to build capacity, ensuring peer educators receive comprehensive training supported by appropriate educational materials and ongoing support [13, 14, 17, 24]. Additionally, delivering peer education through home visits or house-to-house outreach, coupled with the provision of preventive services at primary health care centers, can improve accessibility and uptake [29]. Overall, these recommendations emphasise the importance of community collaboration, culturally relevant content, capacity building and accessible delivery methods to maximise the impact of peer education programs.
Discussion
This paper provides a comprehensive analysis of studies employing peer education as a tool for community breast cancer prevention. The rising incidence of breast cancer among women has driven researchers to develop educational interventions aimed at improving knowledge, beliefs and screening uptake.
The first objective of this review was to examine the structure, strategies and delivery methods of peer education programs in community settings. Findings show that peer educators primarily deliver training through group discussions [17, 21–23], supported by videos [13, 17, 18, 21], practical demonstrations [16, 23, 26, 28] and PowerPoint presentations [14, 25]. This aligns with [31], who reported interventions delivered either one-to-one or in groups. The results confirm the transformative role of peer education, especially among marginalised populations. Peer-led models effectively overcome cultural, linguistic and socioeconomic barriers by leveraging trusted community members. The grade or level of English used in the included studies was not explicitly stated; however, all studies employed culturally tailored interpersonal education approaches. This may be because most of the studies were conducted in the United States and Canada, which are Western and high-income settings with relatively homogeneous English language proficiency. In contrast, within the Low- and- Middle Income Country context such as Nigeria, the use of indigenous languages is often more effective for community-based interventions. This is supported by the findings of [32], who reported that during the critical COVID-19 period, health communication delivered in indigenous languages significantly enhanced the population’s understanding and engagement. Dramatic increases in screening rates from under 5% to over 60% in some studies [23, 29] demonstrate its impact. Beyond behaviour change, peer education fosters empowerment and agency among both educators and participants [15, 25]. Effectiveness is enhanced when educators share ethnic, faith or linguistic backgrounds with their audiences, acting as trusted messengers and cultural interpreters [14, 22]. Embedding sessions in familiar settings like churches, mosques or tribal centers and incorporating local art, food and storytelling also increases participation [12, 16]. These findings are supported by [33], who showed peer education improves health-related knowledge, and [34] who found significant gains in adolescent knowledge and behaviours through peer education.
Despite their promise, peer education interventions face challenges. Role confusion among educators in close-knit communities can cause strain, necessitating training that addresses boundary management and ongoing support [25]. Logistical barriers such as transportation and lack of insurance limit participants’ ability to act on education, risking stagnation at awareness without behaviour change. Cultural sensitivities may also restrict discussion of breast health, especially if educators are unprepared [24, 26]. These issues highlight the need for adaptable, context-specific approaches rather than one-size-fits-all models. Successful programs emphasise cultural competence, community ownership and structural support. Also, it is crucial to involve men in the intervention. Studies by [35] revealed that involving men in the intervention produces better results as they provide emotional and psychological support.
Structured and ongoing training, along with mentorship, are essential to maintain program fidelity and educator confidence [17, 25]. This is echoed by [36], who emphasised that peer education and counselling succeed only when organisational factors are well managed and cultural contexts respected. Attention to program structure, management, training, supervision, support, monitoring and retention is critical for effective peer education initiatives. Community collaboration, culturally relevant content, capacity building and accessible delivery methods should be carefully considered when designing peer education models to maximise their impact. Co-creation of intervention materials with community involvement is a collaborative and democratic approach that recognises both community members and professionals as equal partners in developing community-based peer education [37]. This approach has been applied across a variety of healthcare settings and with diverse patient populations to design person-centered interventions that respond to patient-identified needs. Its application in community-based education is similarly expected to enhance relevance, acceptability and effectiveness.
Although most of the studies included in this review were conducted in high- or middle-income countries, their findings can be adapted to lower-resource settings, such as Nigeria. Translation of these interventions requires culturally relevant content, accessible delivery methods and strong community collaboration. Additionally, local health system constraints, resource limitations and factors such as availability of early detection services, transportation challenges and trust in healthcare providers must be considered to ensure program feasibility, acceptability and effectiveness. Incorporating these adaptations can help bridge the gap between evidence from higher-income settings and practical implementation in Nigerian communities, enhancing the relevance and impact of community peer education interventions.
Implications for practice and recommendations
Based on the findings of this review, the following recommendations are proposed:
-
Integrate peer education into community structures. Leveraging women’s groups, religious networks, cooperatives and other established community organisations enhances credibility and participation [23, 25]. Implementation should engage community-embedded peer educators, CHWs, local survivor-led groups, faith-based educators, and existing health structures.
-
Provide structured training, mentorship and supervision. Clear guidance and support reduce role ambiguity and strengthen program delivery [17, 25]. Training should be delivered by program supervisors, research teams, health-education institutions and advisoryboard-guided trainers.
-
Mitigate logistical and cultural barriers. Transportation challenges, stigma, and other contextual barriers [24, 26] can be addressed through flexible, community-based program designs. CHWs, local health facilities and community educators can manage operational challenges, while policymakers address financial and systemic constraints.
-
Adapt evidence-based models to local contexts. Successful interventions from high-income settings should be tailored to align with local health systems and cultural norms. Researchers and program designers should collaborate with local health authorities, community stakeholders and grassroots health workers to ensure feasibility and acceptability.
Limitations
This review was limited by the predominance of studies conducted in high-income countries and methodological constraints such as small sample sizes and cross-sectional designs. These limitations reduce the direct generalizability of findings to low-resource settings. Nonetheless, by synthesising global findings and contextualising their relevance for Sub-Saharan Africa, this review contributes practical insights for adapting peer education locally. Future research should prioritise longitudinal and mixed-method designs in African and other resource-constrained settings to evaluate sustainability, scalability and long-term health outcomes.
Conclusion
This review adopted a narrative approach to examine the role of community-based peer education in breast cancer prevention. Through a systematic search of six databases, studies published between 2010 and 2025 were identified and screened using strict inclusion and exclusion criteria, ensuring a clear focus on peer-led interventions in culturally diverse and low-resource community settings. By incorporating qualitative, quantitative and mixed-methods studies, the review captured a nuanced understanding of strategies, challenges and contextual factors influencing intervention outcomes. Data extraction and thematic analysis enabled the identification of recurring patterns and effective practices. Findings highlight peer education as a culturally adaptable, cost-effective and community-driven approach to improving breast cancer awareness and early detection, particularly among underserved populations. This review also emphasises the importance of system-level considerations, including access to early detection and diagnostic services, proximity of healthcare facilities, affordability and trust in healthcare providers, as these factors influence the success of peer-led interventions. Based on the evidence, several recommendations emerge for policymakers and healthcare professionals: integrating peer programs into primary care and community health structures, establishing structured training and mentorship frameworks for peer educators, providing mechanisms to sustain engagement over time and ensuring adequate funding to maintain program reach and quality. Collectively, these strategies can enhance the effectiveness, scalability and sustainability of community-based peer education programs, ultimately contributing to improved breast cancer outcomes in diverse populations.
Author contributions
Conceptualisation and design: ROO, CMN, GOA, IOO, OA. Literature search: OA, ROO, CMN, IOO, GOA. Manuscript writing and editing: ROO, GOA, FAA, DA, SA, HAG, DA, IOO, CMN. Data Extraction and Synthesis: ROO, GOA, FAA, DA, SA, HAG, DA. Supervision: CMN, OA. Final approval of manuscript: All authors.
Conflicts of interest
The authors declared no conflicts of interest.
Funding
There was no external funding available for this study.
References
1. Bray F, Laversanne M, and Sung H, et al (2024) Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries CA A Cancer J For Clinicians 74(3) 229–263 https://doi.org/ 10.3322/caac.21834
2. Ferlay J, Ervik M, and Lam F, et al (2024) Global Cancer Observatory: Cancer Today (International Agency for Research on Cancer) [https://gco.iarc.who.int/media/globocan/factsheets/populations/566-nigeria-fact-sheet.pdf]
3. Cathcart-Rake E, Ruddy K, and Johnson R (2018) Modifiable risk factors for the development of breast cancer in young women Cancer J 24(6) 275–284 https://doi.org/10.1097/PPO.0000000000000340 PMID: 30480572
4. Albeshan SM, Hossain SZ, and Mackey MG, et al (2020) Can breast self-examination and clinical breast examination along with increasing breast awareness facilitate earlier detection of breast cancer in populations with advanced stages at diagnosis? Clin Breast Cancer 20(3) 194–200 https://doi.org/10.1016/j.clbc.2020.02.001 PMID: 32147405
5. Oboirien MKA (2014) Clinical presentation, prevalence and management of breast cancer in Sokoto, Nigeria J Womens Health Care 3 149 https://doi.org/10.4172/2167-0420.1000149
6. Jedy-Agba E, Mccormack V, and Adebamowo C, et al (2016) Stage at diagnosis of breast cancer in sub-Saharan Africa: a systematic review and meta-analysis Lancet Glob Health 4(12) e923–e935 https://doi.org/10.1016/S2214-109X(16)30259-5 PMID: 27855871PMCID: 5708541
7. Adeomi AA, Adeoye OA, and Asekun-Olarinmoye EO, et al (2014) Evaluation of the effectiveness of peer education in improving HIV knowledge, attitude, and sexual behaviours among in-school adolescents in Osun State, Nigeria AIDS Res Treatment 2014 131756 https://doi.org/10.1155/2014/131756
8. David X, et al (2023) Breast cancer champions: a peer-to-peer education and mobile mammography program improving breast cancer screening rates for women of African heritage Cancer Causes Control 34 625–633 https://doi.org/10.1007/s10552-023-01704-z
9. Anbazhagan S, Shanbhag D, and Antony A, et al (2016) Comparison of effectiveness of two methods of health education on cancer awareness among adolescent school children in rural area of southern India J Fam Med Prim Care 5(2) 430–434 https://doi.org/10.4103/2249-4863.192357
10. Sarıkaya A and Tunamalak A (2019) A method in prevention of cancer: peer education Asian Pac J Cancer Prev 20(8) 2435–2440
11. Sarkar S and Bhatia G (2021) Writing and appraising narrative reviews J Clin Sci Res 10(3) 169–172 https://doi.org/10.4103/jcsr.jcsr_1_21
12. Anderson-Lewis C, et al (2012) Community-based interventions for breast cancer awareness in the South J Health Dispar Res Pract 5(2) 1–14 https://doi.org/10.1186/1471-2458-11-468
13. Baethge C, Goldbeck-Wood S, and Mertens S (2019) SANRA—a scale for the quality assessment of narrative review articles Res Integr Peer Rev 4 5 https://doi.org/10.1186/s41073-019-0064-8
14. Allicock M, Campbell MK, and Valle CG, et al (2017) Peer connect for African American breast cancer survivors: a pilot study J Cancer Educ 32(1) 155–161 https://doi.org/10.1007/s13142-017-0490-4
15. Almeida R, Lopez-Macha A, and Dugatkin T, et al (2021) Community research collaboration to develop a promotores-based hereditary breast cancer education program for Spanish-speaking Latinas Health Educ Res 36(3) 319–336 https://doi.org/10.1093/her/cyab011 PMID: 34113985PMCID: 9115327
16. Ashing-Giwa K, Tapp C, and Rosales M, et al (2012) Peer-based models of supportive care: the impact of peer support groups in African American breast cancer survivors Oncol Nurs Forum 39(6) 585–591 https://doi.org/10.1188/12.ONF.585-591 PMID: 23107852
17. Chilton JA, Downing C, and Lofton M, et al (2013) Circle of sisters: raising awareness of native American women to breast cancer J Health Care Poor Underserved 24(3) 1167–1179 https://doi.org/10.1353/hpu.2013.0116
18. Gu J, Maxwell AE, and Ma GX, et al (2019) Evaluating the training of Chinese-speaking community health workers to implement a small-group intervention promoting mammography J Canc Educ 34(4) 705–711 https://doi.org/10.1007/s13187-018-1361-5
19. Hamlish T, Holzman Castellands T, and Papautsky EL, et al (2023) Assessing the effectiveness of a learning collaborative to build capacity for community-based cancer survivorship navigation JCO Oncol Pract 19 213 https://doi.org/10.1200/OP.2023.19.11_suppl.213
20. Hanson LC, Armstrong TD, and Green MA, et al (2013) Circles of care: development and initial evaluation of a peer support model for African Americans with advanced cancer Health Educ Behav 40(5) 536–543 https://doi.org/10.1177/1090198112461252
21. Hempstead B, Green C, and Briant KJ, et al (2018) Community empowerment partners (CEPs): a breast health education program for African-American women J Community Health 43(5) 833–841 https://doi.org/10.1007/s10900-018-0490-4 PMID: 29488155PMCID: 6110969
22. Maxwell AE, Wang JH, and Young L, et al (2011) Pilot test of a peer-led small-group video intervention to promote mammography screening among Chinese American immigrants Health Promotion Pract 12(6) 887–899 https://doi.org/10.1177/1524839909355550
23. Padela AI, et al (2018) Religious values and mammography intention among American Muslim women J Health Psychol 23(7) 949–961 https://doi.org/10.1177/1090198118769371
24. Torres E, Richman AR, and Schreier AM, et al (2019) An evaluation of a rural community-based breast education and navigation program: highlights and lessons learned J Canc Educ 34 277–284 https://doi.org/10.1007/s13187-017-1298-0
25. Rodriguez NM, Casanova F, and Pages G, et al (2020) Community-based participatory design of a community health worker breast cancer training intervention for South Florida Latinx farmworkers PLoS One 15(10) e0240827 https://doi.org/10.1371/journal.pone.0240827 PMID: 33075111PMCID: 7571710
26. Ahmad F, Ferrari M, and Moravac C, et al (2017) Expanding the meaning of ‘being a peer leader’: qualitative findings from a Canadian community-based cervical and breast cancer screening programme Health Soc Care Community 25(2) 630–640 https://doi.org/10.1111/hsc.12352
27. Sangwan RK, Huda RK, and Panigrahi A, et al (2023) Strengthening breast cancer screening program through health education of women and capacity building of primary healthcare providers Front Public Health 11 1276853 https://doi.org/10.3389/fpubh.2023.1276853 PMID: 38035296PMCID: 10687205
28. Schliemann D, Jamil ASA, and Mohan D, et al (2023) The development and evaluation of a mHealth, community education and navigation intervention to improve clinical breast examination uptake in Segamat Malaysia: a randomised controlled trial PLoS One 18(10) 288437 https://doi.org/10.1371/journal.pone.0288437
29. Soto-Perez-de-Celis E, Smith DD, and Rojo-Castillo MP, et al (2017) Implementation of a school-based educational program to increase breast cancer awareness and promote intergenerational transmission of knowledge in a rural Mexican community Oncologist 22(10) 1249–1256 https://doi.org/10.1634/theoncologist.2017-0063 PMID: 28652281PMCID: 5634772
30. Chigbu CO, Onyebuchi AK, and Ezeonu PO (2017) Impact of community-based health education on cancer screening uptake in rural Nigeria BMC Public Health 17 515 https://doi.org/10.1002/ijgo.12150
31. World Bank (2024) World Bank Income Groups [dataset] (Our World in Data ) [https://archive.ourworldindata.org/20250624-125417/grapher/world-bank-income-groups.html] Date accessed: 10/09/2025
32. King T and Fazel M (2021) Examining the mental health outcomes of school-based peer-led interventions on young people: a scoping review of range and a systematic review of effectiveness PLoS One 16(4) 249553 https://doi.org/10.1371/journal.pone.0249553
33. Dodd S, Widnall E, and Russell AE, et al (2022) School-based peer education interventions to improve health: a global systematic review of effectiveness BMC Public Health 22 2247 https://doi.org/10.1186/s12889-022-14688-3 PMID: 36461024PMCID: 9719233
34. Obiorah KE (2021) The role of Nigerian indigenous languages in COVID-19 discourse J Lang Health 2(2) 43–52 https://doi.org/10.37287/jlh.v2i2.514
35. Soleimani M, Sadeghi M, and Rashidi Fakari F (2018) Effects of model-based interventions on breast cancer screening behavior of women: a systematic review Asian Pac J Cancer Prev 19(8) 2031–2040 [https://doi.org/10.1371/journal.pone.0249553]
36. Topping KJ (2022) Peer education and peer counselling for health and well-being: a review of reviews Int J Environ Res Public Health 19(10) 6064 https://doi.org/10.3390/ijerph19106064 PMID: 35627601PMCID: 9140904
37. Akpor OA, Kolawole ER, and Olorunfemi O, et al (2023) Breast cancer and body image: the roles of the male partner APIK J Internal Med 11(2) 65–69 https://doi.org/10.4103/ajim.ajim_108_21




