Presentation, treatment and clinical outcomes in young multiple myeloma patients treated at a tertiary care centre in a low middle-income country
Tasneem Dawood1, Sahar Fatima Rizvi1, Syed Muhammad Kashif Kazmi2, Saqib Raza Khan3,4,a, Insia Ali1 and Munira Moosajee1
1Division of Medical Oncology, Department of Oncology, Aga Khan University Hospital, Karachi 74800, Pakistan
2Department of Nephrology, National Institute of Kidney and Urological Disease, Karachi 75270, Pakistan
3Division of Medical Oncology, Department of Oncology, Schulich School of Medicine & Dentistry, Western University, London, ON N6A3K7, Canada
4Verspeeten Family Cancer Centre, London Health Sciences Centre, London, ON N6A5W9, Canada
ahttps://orcid.org/0000-0002-3742-534X
Abstract
Background: Multiple myeloma (MM), a plasma cell malignancy, predominantly affects individuals aged 65–74 years. However, its occurrence in younger populations (<55 years) is rare, posing unique challenges. This study explores the clinical presentation, outcomes and treatment regimens for MM patients aged 30–55, aiming to unravel age-specific patterns.
Methods: A retrospective chart review was conducted at Aga University Hospital, Karachi, focusing on MM patients aged 30–55 years. Data included patient demographics, clinical features, treatment modalities and outcomes. Statistical analysis employed STATA version 16.0, incorporating survival estimates, log-rank tests and Cox proportional survival regression models.
Results: This study encompassed 68 confirmed MM patients, categorised by age groups: 30–40 years (13.23%), 41–50 years (44.11%) and 51–55 years (42.64%). Predominantly male (1.3:1 ratio), bone pains were prevalent among all groups, with 51–55 years exhibiting the highest pathological fracture rate. 30–40 years group showed higher renal impairment rates and lactate dehydrogenase levels. Velcade, thalidomide and dexamethasone were commonly used first-line regimens in the entire cohort in 41.17% of patients, closely followed by cyclophosphamide, bortezomib and dexamethasone in 29.41%. Partial response was predominant in the 30–40 years group, while other age groups showed varied responses. The younger patients demonstrated lower deep treatment response rates than their older counterparts. Progression-free survival was 37, 52 and 45 months orderly in each group, with a p-value of <0.001. The median overall survival (OS) for the entire group was 50.6 months (4.2 years), with OS rates of 77.8% (CI: 95%), 90.0% (CI: 95%) and 86.2% (CI: 95%), respectively, with a p-value of <0.001. Median OS in months was 45, 55.5 and 52, with a p-value of 0.08.
Conclusion: This single-center study sheds light on younger MM patients' unique challenges and treatment patterns. Despite the rarity of this age group's affliction, the findings underscore significant differences in clinical presentations, treatment responses and outcomes compared to the typical elderly MM population. The study highlights the importance of tailored approaches in managing MM across different age brackets, emphasising the need for further research to optimise therapeutic strategies and improve prognosis in this distinct patient cohort.
Keywords: multiple myeloma, young patients, clinical characteristics, treatment patterns, survival outcomes
Correspondence to: Saqib Raza Khan
Email: saqibrazakhan1994@gmail.com
Published: 29/08/2025
Received: 14/01/2025
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Multiple myeloma (MM) is characterised by the proliferation of clonal plasma cells in the bone marrow, and this results in various complications such as bone destruction, renal impairment, anemia and hypercalcemia [1]. MM has been recognised as a disease predominantly affecting the elderly, with the highest incidence reported in individuals aged 65 to 74 years. The risk increases with age, reaching over 40 cases per 100,000 among those over 80. The median age at diagnosis is approximately 69 years. However, MM isn't limited to older adults; although it's rare, younger people can also develop the disease. Around 10% of MM cases are found in individuals under 50 and only 2% in those under 40 [2–4]. This younger group of patients faces unique challenges and needs different treatment strategies than older patients.
The uncommon occurrence of MM in younger patients (under 55 years old) makes it challenging to fully understand its clinical behaviour and devise ideal treatment protocols. Younger MM patients often have different disease characteristics, presentation and response to therapy compared to older patients [5]. For example, younger patients usually have fewer comorbidities, better performance status and may tolerate aggressive treatments better; these differences can impact their clinical outcomes and survival rates. Additionally, young patients face significant impacts on their productive years, including prolonged treatment toxicity and unique challenges related to symptom burden, overall life impact and financial strains [5]. The reduction in life expectancy for these patients can be significant, up to 36 years for those under 40 and 27 years for those aged 40–49 [6, 7].
Despite significant advancements in treatment, MM remains a challenging and mostly incurable disease [8–11]. Current treatment strategies focus on controlling the disease, relieving symptoms, preventing organ damage, improving quality of life and prolonging survival. Over the past few decades, the introduction of novel therapies—such as proteasome inhibitors (e.g., bortezomib and carfilzomib), immunomodulatory drugs (e.g., thalidomide, lenalidomide and pomalidomide) and monoclonal antibodies (e.g., daratumumab and elotuzumab)—has transformed the management of MM, leading to improved survival rates. Standard treatment regimens frequently include a combination of these novel agents with corticosteroids and chemotherapy, often tailored to the patient's condition and disease stage.
Autologous hematopoietic stem cell transplantation (AHSCT) remains a cornerstone of therapy for transplant-eligible MM patients, particularly younger individuals who can better tolerate intensive treatment. Despite improvements in progression-free survival (PFS) and overall survival (OS), relapses remain common due to residual disease. Whether following AHSCT or used in non-transplant settings, maintenance therapy aims to prolong and deepen the responses achieved through initial treatment [12].
Treatment choice often depends on various factors, including disease stage, cytogenetic abnormalities and patient comorbidities. For younger patients, the aim is to achieve the deepest possible response, as achieving a complete response (CR) or stringent complete response (sCR) is associated with prolonged PFS and OS. The goal for younger patients should be to enhance long-term outcomes while minimising treatment-related side effects. However, the best treatment approach for younger MM patients is still an active area of research.
In younger patients, the survival rates tend to be better than older patients, likely due to their ability to undergo aggressive treatments and overall better health status. However, despite these advantages, younger MM patients face a significant disease burden and the potential for long-term complications related to both the disease and its treatment.
Young MM patients are underrepresented in the literature and often overshadowed by older cohorts in clinical trials. Few studies have specifically addressed the clinical characteristics and outcomes of younger MM patients, with most research comprising case reports or small cohorts over several years [5, 13]. The lack of comprehensive studies, with the rapid advancements in therapeutic, diagnostic and biological understanding, underscores the need for a detailed approach to treating this subpopulation. Given this, our study aims to provide valuable insights into disease biology and optimal treatment strategies for this distinct and often overlooked subgroup of MM patients [9, 10].
Methods
This retrospective study was done at the Aga University Hospital in Karachi. The study population comprised young individuals with symptomatic MM from ages 30–55. For the study analysis, they were grouped into ages 30–40, 41–50 and 51–55 years. Patients in the smoldering/asymptomatic phase of MM and those deemed extremely ill to undergo treatment were excluded.
Retrospective data encompassing 2012–2020 were extracted from the medical records of all patients diagnosed with MM within our institution. A structured pre-formed proforma guided the systematic collection of pertinent variables, ensuring a comprehensive and standardised approach to the dataset. STATA version 16.0 was employed for data analysis, involving descriptive statistics for continuous and categorical variables. Mean and standard deviation summarised continuous variables and frequency counts/percentages reported categorical ones. Kaplan–Meier estimates and the log-rank test assessed survival function, while a Cox proportional survival regression model was used for comprehensive analysis. Initial univariate analysis gauged variable significance (<0.25), followed by multicollinearity checks. Significant variables, free of multicollinearity, underwent multivariable analysis (<0.05), including scrutiny for plausible interactions.
Results
A total of 68 patients with a confirmed diagnosis of MM were included in this analysis. The patient population was stratified by age group, of which 9 (13.23%) patients were 30–40 years of age (Group 1), 30 (44.11%) patients were 41–50 years of age (Group 2) and 29 (42.64%) were aged 51–55 years (Group 3). The median ages in each age group were 35, 47.5 and 54 years, respectively. There was a male predominance with a male-to-female ratio of 1.3:1 in the entire cohort, with a much higher ratio in group 1 of 8:1. Bone pains (62/68 – 91.17%) were the most common presenting symptom in all three groups. The rate of pathological fracture was the highest in group 3 (12.5% versus 66.6% versus 81.25%, p = 0.29), though the difference between groups 2 and 3 was not statistically significant. Group 1 had higher rates of renal impairment than groups 2 and 3 (p = <0.01), as well as renal failure (55.6% versus 40% versus 34.5%). Lactate Dehydrogenase (LDH) was also significantly higher in Group 1 than in 2 and 3 (447 versus 307 versus 368 U/L p value <0.001). There were no significant differences in gender, hemoglobin levels, calcium levels, heavy or light chain restriction or International Staging System (ISS) stage. Around 40% of patients in all groups were diagnosed with Stage III. IgG myeloma was more common than non-IgG myeloma in each group (Table 1).
Most of the patients underwent treatment with novel agents. Velcade, thalidomide and dexamethasone (VTD) were the most common induction treatment of choice for the entire cohort, received by 41.17% of the patients, followed by cyclophosphamide, bortezomib and dexamethasone (CyBorD) in 29.41% (Table 2). Treatment selection was guided by a combination of factors, including drug availability, cost considerations, institutional protocols and national guidelines. These determinants played a key role in shaping the therapeutic approach.
Regarding the response assessment after induction treatment, as shown in Table 2, a partial response (PR) was demonstrated in 77.8% of the patients and no very good partial response (VGPR), CR or sCR was observed in group 1 and progressive disease (PD) was observed in 22.2%. For group 2, PR, VGPR and CR sCR were observed in 53.3%, 10%, 6.7% and 6.7%, respectively, and PD was observed in 23.3% of the patients. In group 3, PR, VGPR, CR and sCR were observed in 55.2%, 5%, 5% and 3.5%, respectively, and PD in 6.9%. Out of the 68 patients, only 6 (8.8%) underwent transplant. Most (80%) patients received maintenance treatment, as shown in Table 2. The overall response rate post-induction (ORR: CR/VGPR/PR/sCR) was similar in the first two groups, 77.8% and 76.7%, but significantly higher in group 3 (93.1%).
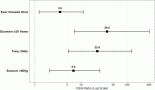
The median follow-up duration for the entire cohort was 57 months. PFS was significantly longer for groups 2 and 3 compared to group 1, with a median PFS of 37 months for group 1, 52 months for group 2 and 45 months for group 3 (p < 0.001), as shown in Table 3. The median PFS for the entire cohort was 44.4 months (p = < 0.001) (Figure 1). The median OS in months for each group was 45, 55.5 and 52, respectively (p = 0.08) (Table 3, Figure 2a). The median OS for the entire population was 50.6 months (4.2 years) (Figure 2b), with OS rates of 77.8%, 90.0 % and 86.2%, respectively, with a (p = <0.001) (Table 4).
Table 1. Patient characteristics associated with MM (n = 68).
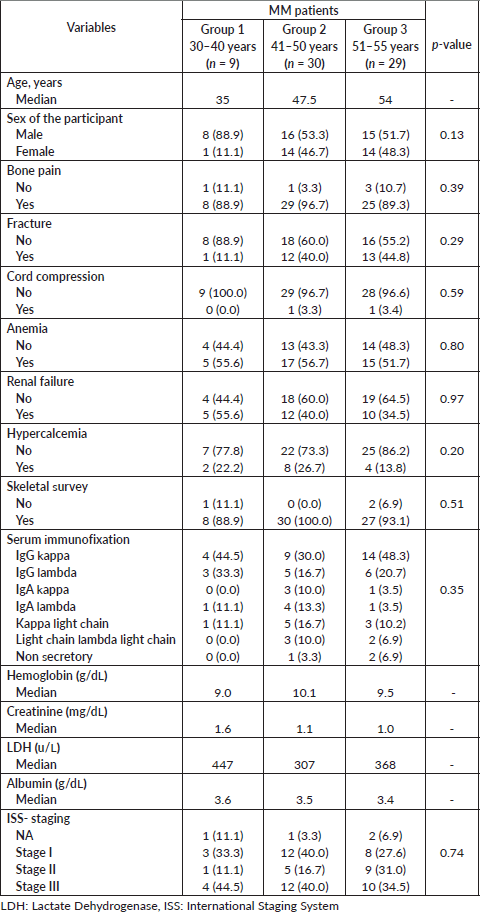
Table 2. Treatment pattern and responses in patients with MM (n = 68).
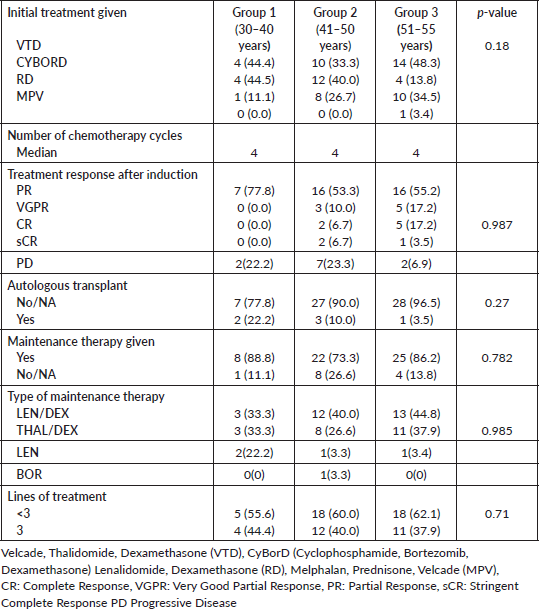
Table 3. Combined survival outcomes by age group in MM patients.
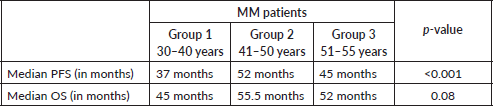
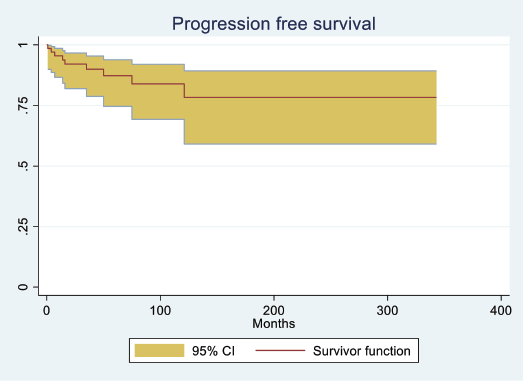
Figure 1. PFS (in months) for the entire cohort of MM patients.
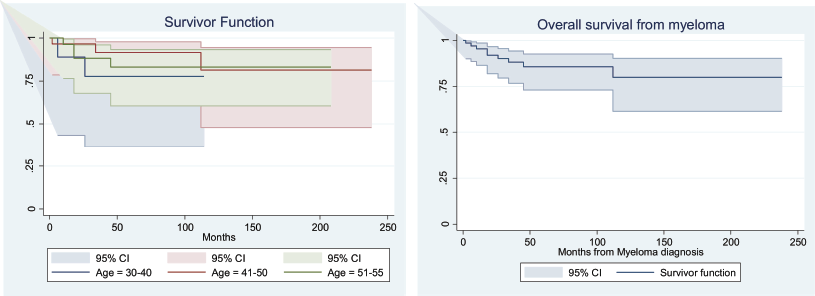
Figure 2. (a): OS (in months) for MM patients in different age groups. (b): OS (in months) for the entire cohort of MM patients.
Table 4. Survival rate (%) stratified on age group.
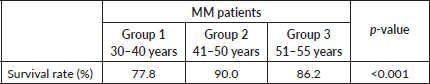
Discussion
The present study investigates the presentation, clinical outcomes and treatment regimens utilised in young patients diagnosed with MM. Since MM is rare in young individuals, a focused approach is required to understand this age group's specific patterns and challenges. The median age of diagnosis for MM is commonly reported to be between 65 and 74 years, making the inclusion of younger patients, aged 30–55 years and a distinctive aspect of this research.
Regarding clinical characteristics and outcomes, this study included 68 patients younger than 55 with a median follow-up of 57 months. Similar studies focusing on young myeloma patients have included comparable participant populations. For instance, a study enrolled 61 patients under 60 years of age, while Yanamandra et al [14] had 40 patients under 40 and Jurczyszyn et al [15] investigated 52 patients under 30. Some notable findings concerning patient characteristics and disease presentation were observed across different age groups. Renal failure was more prevalent among younger patients (30–40 years) in our study than in groups >40 years. While Veerendra et al [16] reported renal failure in 17.2% of younger MM patients and 35.8% of the elderly, their study did not directly compare age groups within the same analytical framework as ours [16]. Additionally, the incidence of pathological fractures was lower in the younger age category in our study. At the same time, Butler et al [17] found that pathological sternal fractures are more common in younger myeloma patients with thoracic compression fractures [17]. These observations suggest age-specific variations in disease presentation.
Our analysis of treatment regimens showed that VTD was the most frequently used first-line regimen, followed closely by CyBorD. Various studies, such as those by Leiba et al [18] and Moreau et al [19] have also highlighted the superiority of VTD therapy in achieving deeper responses. The median OS for the entire cohort in our study is 50.6 months. In comparison, reviews of similar studies suggest that the median OS for MM patients ranges widely from 7 months to over 76 months, depending on factors such as age, treatment regimen and disease stage [13, 19–21]. Distinct OS rates were observed among different age groups in our study. Notably, the 30–40 age group exhibited decreased OS and PFS compared to patients aged 41–55.
In contrast, Jurczyszyn et al [22] demonstrated that younger myeloma patients aged 21–40 have better OS than those aged 41–60, although this survival advantage diminishes in more advanced stages. Despite generally favourable prognoses in some malignancies, younger patients in our study exhibited poorer OS, challenging older analyses suggesting better survival rates for those younger than 50 years [23]. This emphasises the complex and multifactorial nature of MM outcomes.
The treatment patterns in this study indicate that a relatively low percentage of patients undergoing transplants (8.8%) raises questions about the comprehensive management of young myeloma patients. In contrast, other studies show significantly higher transplant rates in young MM patients; notably, Caulier et al [24] found that 25% of young patients had allogeneic stem cell transplantation, and Aytan et al [25] reported 83.9% of young patients undergoing transplants. The low transplant rates in our study may reflect survivorship-related issues such as financial burden, infertility, risks of secondary malignancies and other factors influencing treatment decisions in this population.
The limitations of this study include its retrospective nature and relatively small sample size. The data sparsity made it difficult to conduct thorough univariate and multivariate analyses, indicating a need for larger studies to validate our findings. Additionally, the study did not explore specific genetic or molecular markers, which could provide valuable insights into the heterogeneity of myeloma in young patients.
Despite these limitations, this study sheds light on the unique characteristics of MM in young individuals. The observed age-specific differences in clinical presentation, treatment patterns and outcomes emphasise the importance of developing tailored therapeutic approaches for this population. The findings also point to significant challenges, such as a higher incidence of renal failure and reduced survival rates in the 30–40-year-old age group, which merit further investigation and should be considered when designing personalised treatment strategies for young myeloma patients.
In recent years, the treatment landscape for MM has evolved significantly with the advent of novel therapies that have improved patient outcomes. These include proteasome inhibitors, immunomodulatory drugs, monoclonal antibodies and chimeric antigen receptor T-cell therapy [26, 27]. These advancements offer promising avenues for addressing MM's complex and heterogeneous nature, particularly in younger patients who may benefit from more aggressive and targeted approaches. Ongoing research into the integration of these novel therapies and the exploration of specific genetic and molecular markers holds the potential to further enhance the precision and effectiveness of treatments for young myeloma patients.
Conclusion
This single-center study sheds light on younger MM patients' unique challenges and treatment patterns. Despite the rarity of this age group's affliction, the findings emphasise significant differences in clinical presentations, treatment responses and outcomes compared to the typical elderly MM population. The study highlights the importance of tailored approaches in managing MM across different age brackets, emphasising the need for further research to optimise therapeutic strategies and improve prognosis in this distinct patient cohort.
List of abbreviations
CR, Complete response; CRAB criteria, Calcium elevation, renal insufficiency, anemia, bone lesions; CyBorD, cyclophosphamide, bortezomib, dexamethasone; ISS, International Staging System; LDH, Lactate dehydrogenase; LEN/DEX, Lenalidomide/Dexamethasone; MM, Multiple myeloma; MPV, Melphalan, prednisone, velcade; NA, Not applicable; OS, Overall survival; PD, Progressive disease; PFS, Progression-free survival; PR, Partial response; R-ISS, Revised International Staging System; sCR, Stringent complete response; THAL/DEX, Thalidomide/Dexamethasone; VGPR, Very good partial response; VTD, Velcade (Bortezomib), thalidomide, dexamethasone.
Acknowledgment
The authors would like to thank Salman Muhammad Soomar, who worked as a research instructor in the Department of Medicine at the Aga Khan University Hospital, for his efforts to help us establish the initial database of this research project.
Conflicts of interest
All the authors declare no competing interest.
Funding
No funding is available.
Consent for publication
Not applicable.
Ethics approval and consent to participate
The Aga Khan University Hospital Ethical Review Committee (AKUH-ERC) approved our study. Due to the study's retrospective nature, the Ethical Review Committee of Aga Khan University Hospital, Karachi, Pakistan, waived the need for informed consent.
Availability of data and materials
The data that has been used is confidential. The datasets are available from the corresponding author.
Disclosure
Artificial intelligence tools were not used in the writing or preparation of this manuscript. The authors generated all the content.
Author contributions
TD, SK: Conceptualisation, Writing, Performing the experiment, contributing reagents, analysing and interpreting the data.
SKK: Contributed reagents and analysed the data.
SFR, IA: Perform the experiment, contribute reagents and analyse and interpret the data.
MM: Conceptualisation. Perform the experiment and supervise the manuscript.
TD, MM: Conceived and designed the experiments.
References
1. Baloch SS, Khan SR, and Tariq M, et al (2023) Multiple myeloma and its rare paraneoplastic manifestations simmering under the surface Pathol Res Pract 248 154689 https://doi.org/10.1016/j.prp.2023.154689 PMID: 37478520
2. Costa LJ, Brill IK, and Omel J, et al (2017) Recent trends in multiple myeloma incidence and survival by age, race, and ethnicity in the United States Blood Adv 1(4) 282–287 https://doi.org/10.1182/bloodadvances.2016002493
3. Turesson I, Bjorkholm M, and Blimark CH, et al (2018) Rapidly changing myeloma epidemiology in the general population: Increased incidence, older patients, and longer survival Eur J Hematol 101(2) 237–244 https://doi.org/10.1111/ejh.13083
4. Blimark CH, Turesson I, and Genell A, et al (2017) Outcome and survival of myeloma patients diagnosed 2008–2015. Real-world data on 4904 patients from the Swedish Myeloma Registry Haematologica 103(3) 506 https://doi.org/10.3324/haematol.2017.178103 PMID: 29217784 PMCID: 5830385
5. Tanguay M, Dagenais C, and LeBlanc R, et al (2023) Young myeloma patients: a systematic review of manifestations and outcomes Curr Oncol 30(6) 5214–5226 https://doi.org/10.3390/curroncol30060396 PMID: 37366879 PMCID: 10297423
6. Van der Poel M, Oerlemans S, and Schouten H, et al (2015) Elderly multiple myeloma patients experience less deterioration in health-related quality of life than younger patients compared to a normative population: a study from the population-based PROFILES registry Ann Hematol 94 651–661 https://doi.org/10.1007/s00277-014-2264-0
7. Ludwig H, Bolejack V, and Crowley J, et al (2010) Survival and years of life lost in different age cohorts of patients with multiple myeloma J Clin Oncol 28(9) 1599–1605 https://doi.org/10.1200/JCO.2009.25.2114 PMID: 20177027
8. Elbezanti WO, Challagundla KB, and Jonnalagadda SC, et al (2023) Past, present, and a glance into the future of multiple myeloma treatment Pharmaceuticals 16(3) 415 https://doi.org/10.3390/ph16030415 PMID: 36986514 PMCID: 10056051
9. Hydeman JA, Uwazurike OC, and Adeyemi EI, et al (2019) Survivorship needs of adolescent and young adult cancer survivors: a concept mapping analysis J Cancer Surviv 13 34–42 https://doi.org/10.1007/s11764-018-0725-5 PMID: 30604138 PMCID: 6699632
10. Devine H and Verina D (2017) Young adults with multiple myeloma Seminars in Oncology Nursing vol 33 no 3 (Philadelphia: WB Saunders) pp. 316–331 https://doi.org/10.1016/j.soncn.2017.05.007
11. Dima D, Jiang D, and Singh DJ, et al (2022) Multiple myeloma therapy: emerging trends and challenges Cancers 14(17) 4082 https://doi.org/10.3390/cancers14174082 PMID: 36077618 PMCID: 9454959
12. Gandolfi S, Prada CP, and Richardson PG (2018) How I treat the young patient with multiple myeloma Blood 132(11) 1114–1124 https://doi.org/10.1182/blood-2017-05-693606 PMID: 29967130
13. Puertas B, González-Calle V, and Sobejano-Fuertes E, et al (2023) Novel agents as main drivers for continued improvement in survival in multiple myeloma Cancers 15(5) 1558 https://doi.org/10.3390/cancers15051558 PMID: 36900349 PMCID: 10000382
14. Yanamandra U, Saini N, and Chauhan P, et al (2018) AYA-myeloma: real-world, single-center experience over last 5 years J Adolesc Young Adult Oncol 7(1) 120–124 https://doi.org/10.1089/jayao.2017.0034
15. Jurczyszyn A, Davila J, and Kortüm KM, et al (2019) Multiple myeloma in patients up to 30 years of age: a multicenter retrospective study of 52 cases Leuk Lymphoma 60(2) 471–476 https://doi.org/10.1080/10428194.2018.1480766
16. Veerendra A, Anand N, and Saxena S, et al Clinical profiles and outcomes of young versus elderly patients with multiple myeloma: a retrospective observational study from a tertiary cancer center in South India Cancer Res Stat Treat 6(3) 392–399
17. Butler JS, Malhotra K, and Patel A, et al (2015) Pathologic sternal involvement is a potential risk factor for severe sagittal plane deformity in multiple myeloma with concomitant thoracic fractures Spine J 15(12) 2503–2508 https://doi.org/10.1016/j.spinee.2015.09.031 PMID: 26407504
18. Leiba M, Kedmi M, and Duek A, et al (2014) Bortezomib‐Cyclophosphamide‐Dexamethasone (VCD) versus Bortezomib‐Thalidomide‐Dexamethasone (VTD)‐based regimens as induction therapies in newly diagnosed transplant eligible patients with multiple myeloma: a meta‐analysis Br J Haematol 166(5) 702–710 https://doi.org/10.1111/bjh.12946 PMID: 24861981
19. Moreau P, Hulin C, and Macro M, et al (2015) Bortezomib, thalidomide and dexamethasone (VTD) is superior to bortezomib, cyclophosphamide and dexamethasone (VCD) prior to autologous stem cell transplantation for patients with de novo multiple myeloma. Results of the prospective IFM 2013-04 trial Blood 126(23) 393 https://doi.org/10.1182/blood.V126.23.393.393
20. Facon T, Dimopoulos MA, and Dispenzieri A, et al (2018) Final analysis of survival outcomes in the phase 3 FIRST trial of up-front treatment for multiple myeloma Blood 131(3) 301–310 https://doi.org/10.1182/blood-2017-07-795047 PMCID: 5774211
21. Kim SJ, Kim K, and Kim BS, et al (2009) Clinical features and survival outcomes in patients with multiple myeloma: analysis of web-based data from the Korean Myeloma Registry Acta Haematol 122(4) 200–210 https://doi.org/10.1159/000253027 PMID: 19887776
22. Jurczyszyn A, Nahi H, and Avivi I, et al (2016) Characteristics and outcomes of patients with multiple myeloma aged 21–40 years versus 41–60 years: a multi‐institutional case‐control study Br J Haematol 175(5) 884–891 https://doi.org/10.1111/bjh.14328 PMID: 27682187
23. Rosko A, Giralt S, and Mateos MV, et al (2017) Myeloma in elderly patients: when less is more and more is more American Society of Clinical Oncology Educational Book vol 37 (Alexandria: American Society of Clinical Oncology. Annual Meeting) p 575 https://doi.org/10.1200/edbk_175171
24. Caulier A, Roussel M, and Morel P, et al (2021) Epidemiological landscape of young patients with multiple myeloma diagnosed before 40 years of age: the French experience Blood 138(25) 2686–2695 https://doi.org/10.1182/blood.2021011285 PMID: 34479366
25. Aytan P, Yeral M, and Gereklioglu C, et al (2018) Survival outcomes of young multiple myeloma patients: a single center experience Blood 132 5766 https://doi.org/10.1182/blood-2018-99-118516
26. van de Donk NW, Usmani SZ, and Yong K (2021) CAR T-cell therapy for multiple myeloma: state of the art and prospects Lancet Haematol 8(6) e446-e461 https://doi.org/10.1016/S2352-3026(21)00057-0 PMID: 34048683
27. Zhang X, Zhang H, and Lan H, et al (2023) CAR-T cell therapy in multiple myeloma: current limitations and potential strategies Front Immunol 14 1101495 https://doi.org/10.3389/fimmu.2023.1101495 PMID: 36891310 PMCID: 9986336